How COVID-19 has put a strain on Ghana’s anti-TB programme
It all started six months ago when Karima (not her real name) started coughing but mistook it for a simple case of flu. Even though Karima has a form of Tuberculosis (TB) which has been resistant to different drugs – known as Multidrug-resistant TB (MDR-TB), she said "this cough was different."
MDR-TB is a particular type of drug resistant TB where the TB bacteria that a person is infected with is resistant to two of the most important TB drugs, Isoniazid (INH) and Rifampicin (RMP). If bacteria are resistant to certain TB drugs, the drugs do not work.
“My elder sister took me to a clinic and l was given antibiotics and syrup for the cough but after two weeks there was no improvement,” Karima said.
Her doctor then decided to test Karima's sputum for COVID-19 and shortly after, it was confirmed that she had the virus.
Surprised, Karima was then referred to a hospital where she was prescribed treatment.
At the hospital, Karima said she told the health personnel who attended to her that she had TB, an infectious disease that usually affects the lungs and it was an airborne disease.
"I told them l did not know anyone with COVID-19 and neither have l been in contact with anyone with the virus,” she said. They told her how the COVID-19 disease caused by the SARS-CoV-2 virus spreads between people. She learnt that the disease is spread when an infected person is in close contact with another person.
She learnt that the virus can spread from an infected person’s mouth or nose in small liquid particles when they cough, sneeze, speak, sing or breathe heavily and that people can be infected with COVID-19 when the virus gets into their mouth, nose or eyes when they are in direct or close contact (less than one metre apart) from an infected person.
"Then, it occurred to me I might have been infected by someone with COVID-19 during my daily commute. The buses are often poorly ventilated and people squeeze into the vehicles. I could also have been infected at work where it is always congested," she said.
Karima who used to trade in raw Okro in the Odawna Market near the Kwame Nkrumah Interchange in the Greater Accra Region, says when she became ill, it was very difficult to come to work because she felt so ill and she could not stand.
She said eventually, it got better and six months into treatment, she has started speaking to her fellow traders and friends about her experience and told them that if they have any of the common COVID-19 symptoms, they should immediately go to the hospital to get tested and treated.
Karima is one of the18 persons in the Greater Accra Region battling the dual burden of being infected with TB and COVID-19. (There is no data for the other regions in Ghana at the moment. Only the Greater Accra Region collated data on TB and COVID-19).
"I know that TB is curable and preventable and I had hopes for the future. After three months of treatment as a TB patient, the TB symptoms were almost gone because I only had some joint inflammation, and I was taking my medications to ensure I am fully recovered. Then I got hit with the news of being infected with COVID-19. I didn’t know what to do", said a devastated Karima.
In 2020, a total of 210 MDR-TB patients were detected and the World Health Organisation (WHO) estimates in 2019 showed that a total of 1,200 people had MDR.
Health services under strain
Before the outbreak of COVID-19, Ghana's health system was struggling to provide appropriate care to those who needed it, although some improvements have been made over the years.
Since the outbreak of COVID-19, the country is not only facing its usual health challenges, but has to deal with both the direct costs of COVID-19 and the indirect consequences of the virus.
One of the consequences of the virus is Ghana’s anti-TB programme. TB is one of the major killer diseases and can present symptoms similar to COVID-19. Though TB diagnosis and treatment is free of charge in Ghana, it remains a major public health threat. Majority of the cases (81%) are detected at healthcare facilities. Some districts such as the Volta region have high rates of TB which is more dominant in the southern part, with Ketu South having the highest levels of the disease (TB Control, 2017). People with TB have reported experiencing increased stigma due to the symptoms they present which are similar to those of COVID-19. Many of them with these symptoms have been wary of presenting themselves at the health facilities for testing for fear they will be found to have contracted COVID-19. Those with TB are at higher risk of contracting the virus.
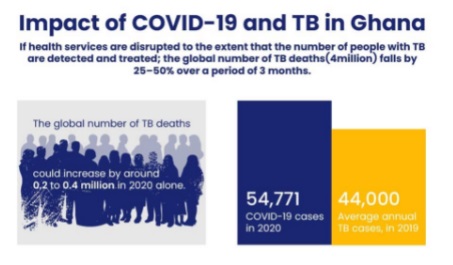
In 2019, an estimated 44,000 people fell ill with TB, and out of this number a total of 15,000 died due to TB. From the total estimated cases in Ghana, males accounted for 51 percent while 31 percent were women and children under 15 years constituted 14 percent.
Although TB incidence rate in Ghana over the past five years shows a slight decline trend, the National Tuberculosis Control Programme (NTCP), in 2019, diagnosed and provided treatment for 15,000 TB patients.
The Programme Manager of the NTCP, Dr Yaw Adusi-Poku says about 66 percent representing 29,000 of TB patients remain undiagnosed in Ghana. Currently, there is limited evidence on whether COVID 19 increases risk of TB reactivation or not. However, Dr Adusi-Poku says COVID-19 can potentially promote the development of active TB disease among COVID-19 patients with latent TB.
He explains that both TB and COVID-19 attack the lungs and treatment outcomes for co-infected patients for the two diseases will be difficult as compared to patients without dual infection.
"Patients with dual infection are highly likely to die as compared to single infection," he said.
To address the treatment and care of TB patients, he said the Programme provides TB diagnosis and treatment free of charge in all government and some private health facilities in Ghana.
Also, to increase access to TB diagnostic tests, the programme established a sputum referral system from 1,000 periphery facilities to 126 GeneXpert testing sites where the patient will not have to travel to the testing site. This is because through the Ghana post courier services the samples can be picked and sent to the testing site for diagnosis. MDR TB patients now have to receive treatment in their district as the programme has decentralized the treatment at regional and district level.
In an attempt to reduce the prevalence of TB in Ghana, the National Tuberculosis Control Programme introduced a symptom-based screening tool (SBS tool) for active case finding. This is where community health workers are trained in the use of the tool to carry out house-to-house screening to detect those with TB. Other methods of detecting TB is the screening that is usually done during the community durbars — public gatherings convened by traditional leaders to consult with their people. However durbars have not been held due to the COVID-19 restrictions that banned public gatherings.
Ghana is implementing Community Directly Observed Treatments (DOTS) to ensure that patients have access to treatment anywhere they are found. DOTS is recommended by the World Health Organization as the “the most cost-effective way to stop the spread of TB in communities with a high incidence by curing it and it is the best curative method for TB”.
DOT involves diagnosis by sputum-smear microscopy and medication given under direct observation and supervision by health care workers to ensure drugs are taken at the right time. But this means it is resource intensive and expensive, making its implementation in low-resource settings difficult.
Digital technology
In Ghana, the use of SMS reminders to patients to take their medication is not as widespread as not everyone has a phone. However, there are opportunities that digital technologies can present to reduce the numbers of those affected and infected by TB. For example, digital health tools such as video (virtual) observation therapy was introduced last year in Eswatini (formerly Swaziland) to reduce the risks MDR TB patients face when accessing medicines at health facilities. The patients film themselves while taking their medicines under the supervision of a community health worker or member. They are provided with a smartphone which is equipped with a secure application through which they can send the video to the healthcare worker. The nurse checks the video and follows up with the patient if there is a problem or if the video does not arrive. This kind of intervention is however not possible in many regions of Ghana where the availability of broadband internet and affordable smartphones is still a big challenge.
The VOT is not a ‘magic bullet’ as it cannot replace the face-to-face interaction with health professionals but it can help case workers ensure their patients adhere to the treatment, reduce the costs that patients have to incur to make frequent visits to hospitals and minimise the stigma that they face from frequent visits by community health workers ensuring they are taking their medication.
Other digital health technologies include Wirelessly Observed Therapy, a device developed by Proteus Digital Health that consists of an edible ingestion sensor and an external wearable patch, which, when it is paired with a mobile device, can detect and record when patients take their medicine.
When patients take their pills, the ingestion event is recorded and uploaded to a secure internet server, so health care workers can remotely confirm that pills were taken. The ingestions can be followed in real time and there’s no limit to the number of patients health care workers can monitor.
Voices
The National Secretary of the TB Voice Network, Mr Jerry Amoah-Larbi, is a trained accountant but now works as an advocate for TB patients. This is after he became infected and affected by TB in 2010.
Following his recovery, Mr Amoah-Larbi has been involved in advocacy, communication and social mobilization for TB.
He says in 2020, an estimated 15,000 persons were diagnosed with TB as against the expected 44,000 in line with the World Health Organisation and Ghana Health Service survey in 2010 which concluded that out of every 100,000 persons in Ghana, an estimated 144 gets infected every year.
He said the number of people diagnosed with TB last year was below the estimated figure because of a number of factors including lack of access to health centres, fear of stigmatisation, and poverty.
“Because only 15,000 persons were diagnosed, it means, about 30,000 infected persons are in our communities who are spreading the disease," he says.
Based on these statistics, Mr Amoah-Larbi estimates that more Ghanaians are dying from TB than COVID-19. “Every two minutes people are dying from TB! More should be done to prevent the spread of TB even as focus is on stopping the spread of COVID-19!” he says.
He suggests that any person who has been exposed to TB in any way should be placed on compulsory medication for at least three months. "This means we do not have to wait for an exposed person to show symptoms before we start treatment."
Mr Amoah-Larbi said since the outbreak of COVID-19 the number of persons diagnosed of TB has gone down since people with symptoms suspected to be TB are shying away from getting tested.
"This development has consequences. It will affect plans of meeting the global target of ending TB by 2030," he says.
And since the outbreak of COVID-19, people who experience symptoms of coughing have been avoiding visiting health facilities because "they are afraid of being diagnosed with COVID-19 and being stigmatised in their communities."
The community awareness programmes have also been suspended meaning that citizens are not only receiving information but the screening programmes to detect those with TB have also been suspended because of the COVID-19 protocols.
The TB Voice Network has 99 volunteers in 33 districts in nine regions in Ghana and were planning on expanding to five more regions. Apart from sharing information about TB, the volunteers are also helping fight stigma surrounding COVID-19 by educating communities to understand the difference between the symptoms of TB and COVID-19 virus.
The volunteers also urge those displaying any symptoms to go for TB testing and diagnosis which is provided free at public and some private health facilities.
And to encourage more TB patients to adhere to the medications and the treatment plan, Amoah-Larbi has been advocating for the government to provide such people with social protection and support. “TB patients must be covered by social protection programmes such as Livelihood Empowerment against Poverty (LEAP) programme during the period they are under treatment to relieve them of some of their financial burdens,” he says.
Under LEAP, the government provides cash and health insurance to extremely poor households across Ghana to alleviate short-term poverty and encourage long term human capital development.
Treatment of TB can span from between six to nine months depending on the type of infection.
"Most patients cannot work and the majority of them are the breadwinners of their families. Although TB treatment is free, the patients have to eat healthy and nutritious foods and they also need financial support to cover their transportation cost from their homes to and from the health facilities where they access health care.
The government must also provide nutrition at the various health centers where TB patients seek treatment,” Amoah-Larbi says.
A patient diagnosed with regular TB needs to take his or her medications for at least six months while MDR TB patients have to continue their treatment for nine months without interruptions. A number of antibodies are combined and if the patient goes on and off medications, he or she may develop resistance.
Interruption in treatment was inevitable when the government instituted lockdown measures to curb the spread of the COVID-19 virus. Health facilities have been giving patients additional medicines to continue treatment at home and minimise hospital visits. However, their most urgent needs —non-medical support including nutritional, economic and psychosocial support have not been met.
The government focus on controlling the spread of the coronavirus has meant that attention to other diseases such as TB has been minimal.
TB patients, particularly those living in informal settlements or in the rural areas who are not able to access the medicines from public health facilities cannot afford to buy the medicines which are extremely costly and beyond the reach of many of the patients.
A 2018 study estimated that the cost of medicines for the treatment of non -MDR TB patients was GH¢2,475 (US$420) while drugs for those with MDR TB the cost was estimated to be GH¢3,794 (US$659.0). The daily minimum wage is GH¢11.82 (US$2.08). Those infected are not able to work which presents additional burdens on families.
Mr Amoah-Larbi said with support from the Global Fund, the government through the Ministry of Health collaborated with NGOs to provide food relief items to a total of 9,700 TB and HIV patients over a two-month period last year. This support has since ceased and TB patients have since been left to their own devices.
The pandemic has adversely affected global plans to end TB by 2030. One of the targets that can be affected is the WHO’s End TB Strategy goal to eliminate catastrophic costs of TB-affected households by 2030.
To prevent dual infection of TB and COVID-19, Mr Amoah-Larbi said there will be the need to strengthen promptness of response to the COVID-19 pandemic and treatment of TB patients in hospitals and health centres.
He advocates the use of appropriate communication strategies, economic support for patients and healthcare workers as essential tools to guarantee TB care and prevent the erosion of all results achieved in recent years in the fight against TB.
"TB can be prevented, diagnosed, treated, and cured. People with TB must not die because they are unable to access diagnosis and life-saving treatment," he said.
