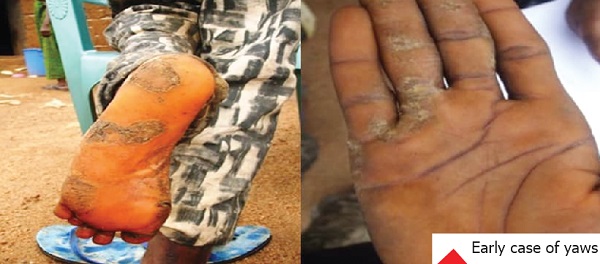
Buruli ulcer, leprosy: Low level awareness increases spread
Comfort Oware of Gboloo-Kofi in the Akuapem North municipality had gone to the farm as usual one early morning last year. While working on the farm, she stumbled over a stump and felt a sharp pain.
Although there was no cut, upon getting home, the 72-year-old farmer realised that the affected area of the foot had begun to itch persistently.
After continuous scratches for a few days, a small sore developed, grew bigger and spread across her sole, creating a wound at a spot.
Ms Oware told the Daily Graphic at Gboloo-Kofi, near Adawso, that it was during one of the numerous visits to health facilities in search of treatment that she was diagnosed of Buruli ulcer, a disease she had no knowledge about.
She shared her story when a team from the Daily Graphic visited the Akuapem North municipality, one of the Buruli ulcer and leprosy endemic areas where the Ghana Health Service (GHS) in collaboration with an international non-governmental organisation (NGO), Anesvad Foundation, had embarked on a start-up project to control Buruli ulcer, eliminate leprosy and eradicate yaws.
It is an endemic district because the two diseases are common there due to the lack of potable water in the affected parts of the district, a contributory factor to the transmission.
The diseases are prevalent where there is inadequate water and where people hardly get water even to bath. They are, therefore, known as water-washed diseases.
Buruli ulcer, especially, is likely to affect people where there is slow moving water bodies and the integrity of the soil is disturbed.
The municipality is one of the 15 selected districts in the country where the GHS and Anesvad are fighting three of the Neglected Tropical Diseases (NTDs).
Ms Oware’s story is similar to that of Peter Ankrah, a retiree from New Asuoyaa, also in the Akuapem North municipality.
For Mr Ankrah, in 2007, he noticed patches of skin that were lighter than his overall skin tone all over his body, a condition known as hypopigmentation.
He did not seek medical attention until somebody spotted it and told him it was one of the symptoms of leprosy.
Mr Ankrah said he still did not see the need for medical help until later in 2019 when he saw his fingers and toes getting deformed, then he recalled the conversation in 2007 that it could be leprosy.
At a health facility, it was confirmed that he had leprosy.
Neglected Tropical Diseases
Leprosy, Buruli ulcer and yaws are among a group of 20 conditions known as Neglected Tropical Diseases (NTDs) which are mainly prevalent in tropical areas such as Ghana, and affect over 1.7 billion people.
The transmission thrives on insanitary environments, especially the lack of potable water.
They are called "neglected," because they generally afflict the world's poorest and historically have not received as much attention as other diseases.
Apart from the three conditions, other NTDS include dengue fever, Guinea worm disease, rabies, trachoma and onchocerciasis.
NTDs cause immeasurable suffering; they debilitate, disfigure and can be fatal. The conditions create cycles of poverty and cost developing nations billions of dollars every year.
NTDs continue to be reported in a number of communities in Ghana, as well as in a number of West African countries.
Poor information on NTDs
Interacting with various people, including patients, health workers, family members of patients, municipal health officers and community leaders, it became clear that there was low awareness that those health conditions still existed, how they presented and the steps to take when one noticed those presentations on one’s body.
This means most of the patients present at the health facility only when the conditions are in their advanced stage, by which time deformities have set in.
Lack of awareness
A Physician Assistant at the Adawso Health Centre, Prince Asiamah, said some people moved from one traditional healer to the other and from one church to another when those conditions first manifested in them because they thought they had been cursed.
Mr Asiamah said some of them went to herbalists where concoctions were applied on the wounds, especially those with Buruli ulcer, and it was only after those interventions failed to bring healing to them that they report to the clinic for treatment.
He said during outreach programmes to endemic communities, they had to talk a lot and make all efforts to establish good rapport with people before those suffering from the diseases would come to them for help.
“Others come when the wound is advanced, has been infected, there are discharges and they are usually in pain. They try to treat it at home but when they see that they are not getting well, then they rush to the facility, by which time the wound is so bad,” a nurse at the Adawso Health Centre, Doris Dede Tetteh, said concerning buruli ulcer.
Unfortunately, seeking treatment late has dire consequences, she explained.
The Programme Manager of the National Buruli Ulcer Control and Yaws Control Programme (NBUYEP) of the GHS, Dr Nana Konama Kotey, said those not treated early for those conditions often suffered long-term functional disabilities.
She explained that early case detection and diagnosis were, therefore, crucial to minimise morbidity and prevent disability.
What are they?
Buruli ulcer and yaws are diseases that affect the skin mainly but could also affect bones, joints and cartilages.
Dr Kotey explained that Yaws formed part of a group of chronic bacterial infections commonly known as the endemic treponematoses. It is caused by a bacterium, treponema pallidum.
The early phase of yaws may present with pain in the bones and joints. There are also ulcers, bony/joint swellings and tenderness.
Buruli ulcer is caused by mycobacterium ulcerans. The organism belongs to the family of bacteria that causes tuberculosis and leprosy.
One is likely to get it where there is slow moving water bodies and where the integrity of the soil is disturbed.
It may start as a painless swelling (nodule), a large painless area of induration (plaque) or a diffuse painless swelling of the legs, arms or face (oedema).
The disease process evolves generally with no pain or fever. When there is pain or fever, it is likely to suggest a super-imposed bacterial infection.
Underlying bones may also occasionally be affected, leading to deformities.
Leprosy, on the other hand, is a chronic, progressive mildly infectious disease, mainly affecting the skin and peripheral nerves.
It can cause progressive and permanent damage of nerves, leading to functional impairments and physical deformities.
The majority of people (95 per cent) who are exposed to leprosy do not develop the disease.
Those at greatest risk are people who have lived in a household-like setting with a person with leprosy over a prolonged period.
Dependent on patient’s cellular immune response, skin rashes of various types may occur and this range from abnormal skin appearance, macules and papules to nodules, plaques and infiltrations. Facial infiltration is referred to as leonine facies.
Prevalence
Suspected cases of yaws recorded across the country in 2016 were 1,497; those for 2017 were 1,917; 7,459 for 2018; 4,694 for 2019; 7,812 for 2020; 3,671 for 2021 and 8,989 from January to May 2022.
For Buruli ulcer, the suspected case trend was 971 for 2011; 571 for 2012; 550 for 2013; 420 for 2014; 275 for 2015; 371 for 2016; 538 for 2017; 877 for 2018; 533 for 2019 and 129 for 2020.
Stigmatisation
Touching on stigmatisation of the conditions, a community Mental Health Officer at the Adawso Health Facility, Alhassan Nuhu, said because of stigmatisation, some patients with the diseases were often reluctant to come to health facility for treatment.
“They think that when they come to the facilities with those conditions, people will laugh at them so they don’t come for treatment,” he said.
For such, he explained that the health workers visited them at home for treatment.
“When the healing process starts, they feel happy to come to the facility just to say hello and to tell us they are now better,” he said.
Ms Oware said some relatives who used to welcome her to their homes suddenly started to act strangely towards her after contracting the disease.
“I have also stopped attending public gatherings not because I feel shy but because I do not want to be looked at differently,” she explained.
For Mr Ankrah, the Daily Graphic learnt that his family had abandoned him since he was diagnosed with leprosy.
A benefactor who has since offered to provide him food, Janet Sarfo, said he was initially spending his whole day, including, spending his night, under a tree in the village under bad weather conditions.
Touched by that pathetic situation, the New Apostolic Church at New Asuoyaa, offered him their premises to live in and that is where he had been ever since.
“He has two children who live in Larteh, grandchildren who live in this village and his wife who resides in the city, but none of them ever pays him a visit,” Ms Sarfo and a volunteer of the programme, Mary Adubea Bekoe, said.
Steps being taken
At the national level, Dr Kotey said under the Anesvad Project, they were raising awareness of the three diseases.
As part of this project, various health workers had been trained on how to treat the disease.
She said various training sessions were also organised for people in communities on how the cases presented themselves and the steps that needed to be taken when they noticed the symptoms.
