
It’s time to talk about safe surgery in Ghana
If you have driven on the streets of Accra recently, you would probably have noticed people weaving through cars at traffic lights carrying signs with pictures of people with different types of medical conditions.
They are seeking donations for treatment and common images, which include children with a cleft lip or club foot, a woman with a facial tumour - conditions requiring surgical treatment.
Advertisement
Sometimes, the people in the photos stand by the side of the road while an individual speaks into a microphone beckoning passers-by to donate.
It can be hard to determine the credibility of these individuals or their organisations, but they are symptoms of a much larger public health problem; the dismal weakness of surgical care in the country.
Surgical condition?
Just the thought of surgery can conjure fear in people’s minds. But surgery is an important medical intervention that is essential in treating a myriad of conditions and preventing death and disability.
Common surgical procedures include caesarean sections, cancer treatment, treating serious injuries and any procedure that requires anaesthetic.
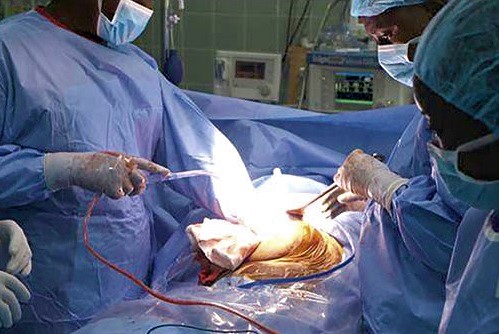
Birth defects are often treatable surgical conditions such as cleft lip and palate or a congenital heart defect.
Surgery has also been used to restore sight for hundreds of millions of people through cataract surgery.
So why does surgery remain in the shadows of public health discourse and policy making in Ghana?
Misconceptions
Two misconceptions may be contributing to surgery’s relatively low profile as a public health issue. First, is the idea that the disease burden of surgical conditions is not as high as other diseases like malaria and HIV/AIDS.
In fact, recent studies show that surgical conditions may lead to more global deaths than malaria, tuberculosis and malaria combined.
Secondly, surgery is perceived to be too costly. This has also been disproven by studies that show that surgical care is as cost-effective as common public health interventions like bednet distribution against malaria, and antiretrovirals for HIV.
In Ghana, surgical care provision seriously fails to meet current needs. Currently, the country carries less than 900 surgical procedures per 100,000 people, significantly below the internationally recommended targets of 5,000 procedures per 100,000.
Children are the least likely to receive surgical treatment; compared to countries like New Zealand, Ghana meets only about seven per cent of children’s surgical needs.
Improving surgical care
The problem in Ghana is not just low numbers of surgeries but also quality. For example, almost 20 per cent of women are estimated to give birth by C-section but maternal mortality is on the rise.
Quality obstetric care is needed to prevent deaths from common complications like haemorrhage.
Ghana also faces a significant shortage of skilled surgical staff. Currently only about 24 per cent of hospitals have specialist surgeons.
According to the World Federation of Societies of Anesthesiologists, Ghana currently has about 110 specialist anesthesiologists for a population of about 26 million people, with most in Accra and Kumasi. The majority of surgical care is provided by non-specialists.
Surgery also places a significant financial strain on families. Although the national health insurance scheme reduces the risk of healthcare impoverishment, one study found that more than half of insured patients seeking surgical care were still not protected from out-of-pocket payments for medicines, laboratory tests and imaging.
The good news is that basic amenities like reliable water and electricity are available at most health facilities.
Nonetheless, surgical teams at district hospitals, where the majority of surgical care is provided, do not have consistent access to operating room infrastructure and supplies as well as imaging services.
Recommendations
Ghana appears to be trailing behind countries like Tanzania, Rwanda and Nigeria who have developed National Surgical Plans as part of their national health strategies.
Ghana could learn from these countries by convening a national dialogue with policy makers, trainers, professional associations, private and public faith-based surgical providers, and other stakeholders with a clear agenda to address the barriers to improved surgical care, especially outside the main cities.
The government should also prioritise the healthcare workforce. While it has launched its largest health infrastructure project ever to construct and rehabilitate 111 health facilities, it must ensure that adequate surgical and hospital staff are trained to provide quality surgical care within these hospitals.
Incentives to retain highly trained healthcare staff are also needed. This is especially important as countries like the United Kingdom and Canada have intensified efforts to recruit healthcare workers from Africa.
Between January and April 2021, over 8,000 foreign-trained nurses reportedly joined the UK’s National Health Service.
Surgery has been a low order issue in public health in Ghana for too long. It is in our best interest to take immediate action to develop and implement policies that will strengthen our surgical system to save thousands of lives and improve the life chances of many thousands more.



