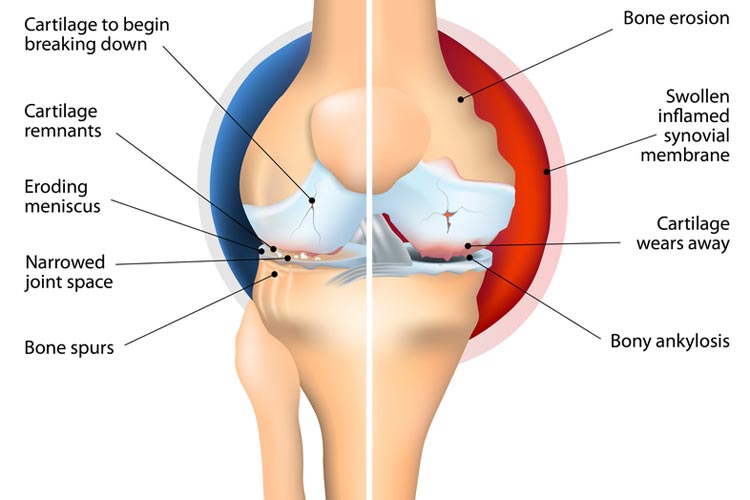
Physio management of rheumatoid
Individuals with rheumatoid arthritis frequently discover that their joints become very stiff and the muscles become weak.
They may also experience loss of movement in the affected joints and therefore have difficulty with carrying out daily activities, such as sitting and getting up from a chair and climbing up and descending the stairs.
Advertisement
Management of rheumatoid arthritis includes physiotherapy, education on joint protection and lifestyle changes.
The physiotherapist assists by educating and encouraging safe stretching and strengthening exercises, to improve movement and strength which eventually results in better function.

The physiotherapist also examines the manner in which the individual performs his/her daily activities whilst maintaining different postures to determine whether there is a need for assistive devices for example to enhance gait.
The physiotherapist assesses the patient on the following components;
• Available movement in all joints
• Postural assessment
• Functional assessment (for example activities of daily living, gait)
• Muscle strength
• Respiratory function (breathing) assessment
Objectives of physiotherapy in the management of rheumatoid arthritis are as follows;
• To prevent disability
• To increase functional capacity
• To provide pain relief
• To provide education
Physiotherapy is frequently used in the treatment of rheumatoid arthritis. Modalities used include cold/warm therapy, splinting and therapeutic exercise.
Education
Physiotherapists educate individuals in the use of assistive devices, joint protection strategies and therapeutic exercises. Joint protection strategies, such as splinting, compressive gloves and assistive devices have beneficial effects in managing the condition.
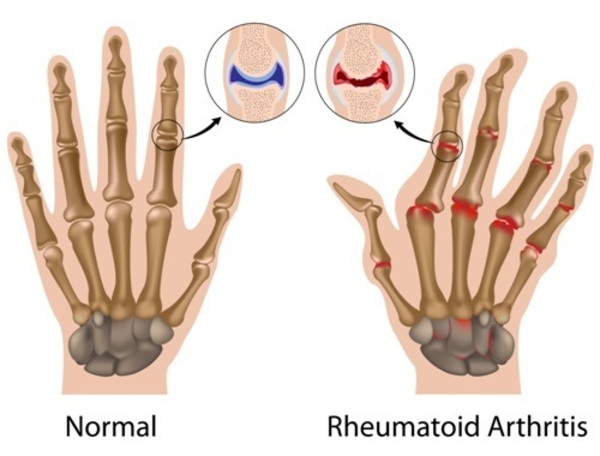
The joints should be at rest during the early stage of the disease. Rest provides pain relief in cases of extensive joint involvement and hence it’s essential to place the joints into rest in a functional position.
Orthosis and splinting are used to diminish pain to support joints, to prevent development of deformities, to prevent joint stress, and to decrease joint stiffness.
Assistive devices may also be used for individuals with rheumatoid arthritis to improve functional ability and independence in daily activities.
Appropriate devices which may be beneficial are anterior walkers, walking sticks etc.
The use of assistive devices also decrease the amount of weight placed on the joint and it also reduces fatigue and pain.
Some individuals may require insoles in their shoes to reduce pain and restore good foot positioning.
Heat/ warm modalities
The application of warm modalities are the most commonly used physical agents in rheumatoid arthritis treatment. Sometimes cold modalities may be used in the early stages of the condition whereas the warm modalities are used in later stages of the condition.
By using heat modalities, pain relief is achieved or reduced. The warm modality is used before exercise for maximum benefit and applied for 15–20 minutes once or twice a day.
Therapeutic exercise
Muscle weakness in individuals with this condition may occur as a result of immobilization or reduction in activities of daily living.

Preservation of normal muscle strength is vital not only for physical function but also for stabilization of the joints and prevention of traumatic injuries.
Strenuous exercises are not advised during the initial stages of the condition but every joint is mobilized at least once each day in order to prevent permanent joint stiffness.
Isometric exercises are used in the early stages to improve or maintain the muscle tone.
Also, stretching and strengthening exercises, aerobic conditioning exercises, and daily activities may be incorporated into the therapeutic exercise.
In later stages of the rheumatoid arthritis, conditioning exercises such as cycling, swimming and walking with adequate resting periods are advised as these exercises increase muscle endurance and improve the general function of the individual.
The writer is a Senior Physiotherapist at the 37 Military Hospital,
[email protected]




