Education to protect tomorrow
“Language matters” is a conscious push in the world of diabetes care these days. One of the key messages of language matters is to recognise that a practitioner is dealing with a "person living with diabetes" and not a "diabetic".
This focuses diabetes care on the person and not just a disease entity. Living with diabetes is probably one of the most complex things to do as it demands lifelong 24/7 attention to achieve desired outcomes.
Advertisement
Diabetes is a chronic progressive disease characterised by high blood sugar and leads to complications in multiple organs over time. Type 2 diabetes mellitus accounts for over 90 per cent of all diabetes, which is the focus of this article.
Last year I shared a brief overview of diabetes which can be reviewed here.
Education on diabetes self-management significantly improves and empowers people living with it to better manage the condition.
This article provides education on Type 2 diabetes in commemoration of World Diabetes Day every November 14.
Preventable
Type 2 diabetes mellitus is preventable and, within the early years, can be forced into remission. Several studies have shown that losing five per cent of body weight or more can prevent diabetes in people with prediabetes.
Other studies have confirmed that more than two-thirds of people living with diabetes can go into remission with 10 per cent body weight loss. Remission means a return to normal blood glucose without the use of medications over a three-month period.
These benefits only remain as long as the weight loss is maintained. Weight loss is achievable with aggressive lifestyle changes, medications or metabolic surgery.
Aggressive lifestyle changes often have a positive impact because increased physical activities can cause the body to use more energy while reducing food intake creates a deficit that can only be replenished by burning stored fats and carbohydrates.
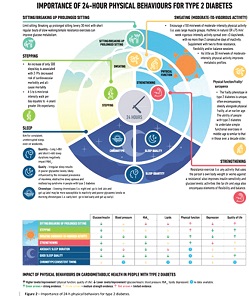
Many activities of an individual affect the control of blood sugar in the body. The image below is from the most recent American Diabetes Association and European Association for the Study of Diabetes (September 2022) consensus on the management of high blood sugars.
It shows the contributions of simple daily activities e.g., breaking up prolonged sitting, walks, sleep, among others, to overall health. (Source : ADA/EASD Consensus Report on Management of Hyperglycemia 2022)
Undiagnosed
Diabetes is usually not diagnosed early. According to the International Diabetes Federation's 10th atlas, about 50 per cent of people living with diabetes worldwide are undiagnosed as of 2021.
Diabetes usually has no symptoms in its early stages.
The classic symptoms of increased thirst, urination, and weight changes usually show up late in the disease process.
In fact, there is evidence that 50 per cent of people diagnosed with diabetes have some complications at the time of diagnosis, emphasising the need for healthy living and appropriate screening. When was your last blood sugar screening test done? What was the result and its interpretation?
Restricted
The person living with diabetes is not restricted to only one kind of food for good blood sugar control. Apart from highly processed foods and refined sugary products, many others can be consumed safely in appropriate quantities.
Vegetables have been shown to better manage blood glucose because of their high fibre and low sugar content. The meals of a person living with diabetes can be planned with an experienced dietician based on preferences, availability and context to include appropriate variety.
Balanced diets are more likely to supply all the body's needs for optimum health.
Dangerous
Doing nothing, especially after diagnosis, is not an option and is too dangerous for you and your family. Many people living with diabetes are unable to make adequate dietary changes, increase physical activities or are too late in the disease process to manage it without medications.
Medications usually are an add-on to these lifestyle changes and work by different mechanisms to control blood sugar.
These medicines could be orals or injectables and do not necessarily indicate the severity or worsening of it.
Specific medicines are chosen based on the agreed targets, patient's preference, cost and potential side effects.
Fortunately, we now have disease-modifying medications in the diabetes world which protect the heart and kidneys aside from the benefits of blood sugar control.
Normalising blood sugar, blood pressure and cholesterol is the surest way to prevent strokes, heart attacks, chronic kidney diseases, blindness, amputations and many more.
Monitoring
Monitoring and feedback are crucial. The person living with diabetes should monitor their weight, physical activity (step count, duration and frequency), blood pressure and blood sugar as agreed. These are key parameters that guide actions, show what works for a particular person and reinforce behaviours over the long term. Checking your blood sugars after meals helps you to choose appropriate foods and quantities for good control.
Regular review with your primary care provider is an opportunity to assess progress, intervene appropriately and strategise for the future.
Consider working with your primary care practitioner to screen for complications annually.
My hope is that after reading this you will make a conscious effort at healthy living and engage in an appropriate screening with a practitioner to protect the future. If you are already living with diabetes, I hope your understanding has increased and will continue to work with your primary care provider to improve your health outcomes.
The writer is a Family Physician with a special interest in Diabetes at the Nyaho Medical Centre; Lecturer, Central University.



